What is Diabetic Retinopathy?
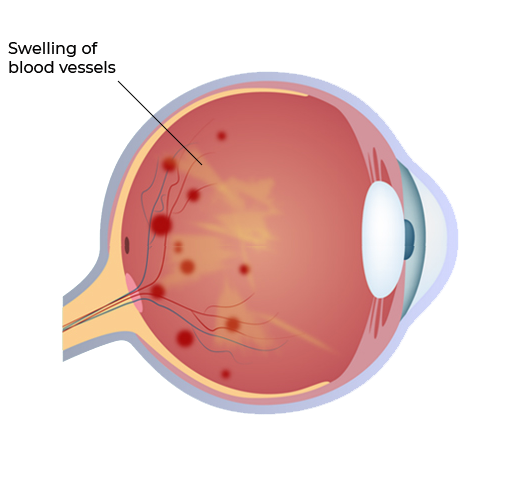
Diabetic retinopathy is a sight-threatning complication of diabetes, which is result of damage to the tiny blood vessels that nourish the retina. They leak blood and other fluids that cause swelling of retinal tissue and clouding of vision. This is "non-proliferative Diabetic Retinopathy". The condition usually affects both eyes.
If the eye disease worsens, areas of the retina may not get enough blood supply to which the eye responds by growth of new blood vessels on the surface of retina. This is termed as "proliferative Diabetic Retinopathy" characterized by complicated problems like "vitreous hemorrhage" (bleeding inside the cavity of the eye) and "tractional retinal detachment". It causes progressive damage to the retina (the light sensitive lining of the eye).
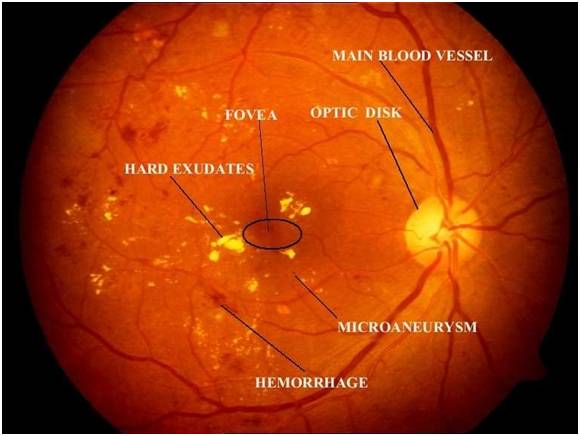
Non-proliferative Diabetic Retinopathy
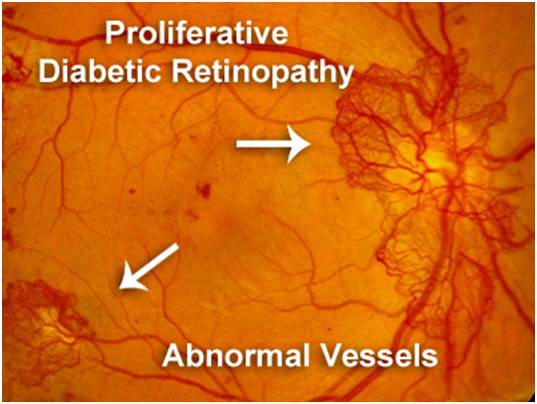
Proliferative Diabetic Retinopathy